You finally got the call. They’re being discharged.
And instead of relief… there’s this quiet panic sitting in your chest.
“What happens now?”
“What am I supposed to do with them all day?”
“What if I miss something?”
I hear these questions from parents every single day.
And if you’ve found yourself searching for something like structured daytime care options because home suddenly feels too unstructured, too quiet, too risky—you’re not overreacting.
You’re responding to a gap no one prepared you for.
You Think Discharge Means Stability
Let’s start here, because this belief creates a lot of pressure.
If your child is being discharged, it feels like they must be okay. Stable enough. Past the worst of it.
But hospitals are designed for crisis stabilization—not long-term healing.
They help your child:
- Get through the most dangerous moments
- Regulate enough to be safe
- Begin initial treatment
But they don’t rebuild daily life.
So when your child comes home, they’re often:
- Emotionally raw
- Easily overwhelmed
- Still unsure how to function outside a structured setting
Discharge doesn’t mean “better.”
It means “ready for the next layer.”
You Expect Home to Replace What the Hospital Provided
This is where things quietly fall apart for a lot of families.
In the hospital, your child had:
- A consistent schedule
- Clinical support throughout the day
- Built-in accountability
- Limited distractions
At home?
None of that exists automatically.
Even with the best intentions, most families can’t recreate that level of structure. And when structure disappears, symptoms often creep back in—not dramatically, but gradually.
Days start to blur. Sleep gets off. Motivation drops. Anxiety or depression finds space again.
This is why many parents begin searching for after hospital mental health support—not because something went wrong, but because something essential is missing.
You Feel Responsible for Holding Everything Together
This one hits deep.
You might be thinking:
- “I need to watch them more closely.”
- “I should know what to say if they spiral.”
- “I can’t let this happen again.”
That pressure can become overwhelming fast.
And here’s the honest truth:
You cannot replace a full care team.
You’re not supposed to carry this alone.
When parents try to become:
- The monitor
- The therapist
- The motivator
- The safety plan
It often leads to exhaustion—and sometimes even pushes the child further away emotionally.
You’re Walking a Tightrope Between Control and Fear
This is one of the hardest emotional balances.
On one side, you want to protect them at all costs.
On the other, you know you can’t lock down their entire world.
So you hover in the middle:
- Checking constantly
- Worrying when they’re quiet
- Second-guessing every decision
Too much control can feel suffocating to them.
Too little structure can feel unsafe to you.
That tension doesn’t mean you’re doing it wrong.
It means you need support that exists outside of the home—where your child can be held safely without it all resting on you.
You Might Not Realize How Disorienting “Normal Life” Feels to Them
Coming home sounds comforting.
But for your child, it can feel like being dropped into open space.
In the hospital, everything was contained. Predictable. Monitored.
At home, suddenly:
- Decisions come back
- Time stretches out
- Internal thoughts get louder
And underneath that, there’s often:
- Shame about what happened
- Confusion about how to move forward
- Fear of slipping back
They may not say any of this out loud.
But you might see it in small ways—withdrawal, irritability, lack of energy, or just not seeming like themselves.
You Expect a Quick Return to “Normal”
This expectation is so common—and so painful when it doesn’t happen.
Parents often hope:
- A few days of rest will help
- A follow-up appointment will stabilize things
- Life will slowly go back to how it was
But recovery doesn’t usually move that fast.
What your child often needs is a transition period—a bridge between crisis care and full independence.
Not constant hospitalization.
Not being left alone all day.
Something in between.
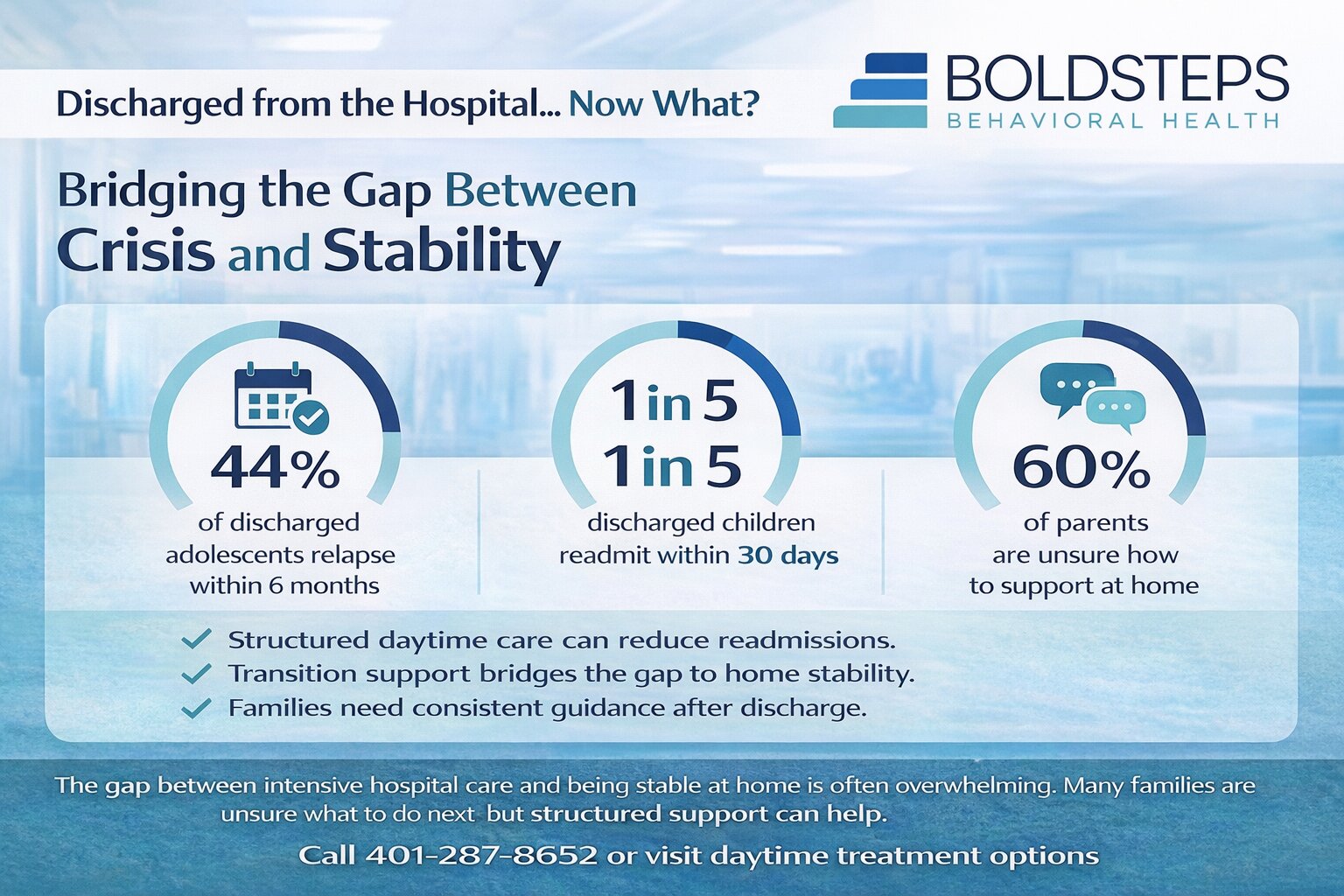
The Gap Between Crisis and Stability Is Where Most Families Struggle
This is the part no one explains clearly.
There’s a gap between:
- Being unsafe (hospital-level care)
and - Being fully stable (independent daily life)
That gap is where your child is right now.
And without the right support in that space, things can feel:
- Unsteady
- Unpredictable
- Emotionally draining for everyone involved
That’s why structured daytime care exists—not as a step backward, but as a bridge forward.
The Hardest Truth: Love Isn’t the Same as Structure
This is not a criticism. It’s a reality.
You can love your child deeply. Show up fully. Be present every moment.
And still not be able to provide what they need right now.
Because what they need isn’t just care—it’s consistency, therapeutic support, and a rhythm that helps their mind stabilize again.
Love creates safety.
Structure creates progress.
They need both.
What Actually Helps in This Phase
Parents often feel like they need a perfect plan.
You don’t.
But there are a few things that tend to make a real difference:
- Consistent daytime engagement so they’re not alone with overwhelming thoughts
- Clinical guidance so you’re not guessing what’s helpful
- A gradual transition back into daily life instead of a sudden drop into independence
Even revisiting structured support—similar to what they experienced during early care—can help rebuild stability without starting over.
And yes, families across Rhode Island often reach this point after discharge. It’s more common than people talk about.
FAQ: What Parents Ask in This Exact Moment
Is it normal to feel scared bringing my child home?
Yes. Almost every parent feels this. You’re stepping out of a controlled environment into uncertainty—it’s a big shift.
How do I know if my child needs more support?
If you’re noticing withdrawal, emotional instability, lack of structure, or just a gut feeling that something isn’t right—that’s worth paying attention to.
Am I supposed to monitor them all day?
No. It’s not sustainable, and it’s not what helps long-term. Support works best when it’s shared—not carried by one person.
What if they resist more help?
That’s common. Many young adults feel overwhelmed or resistant at first. Framing support as structure—not punishment—can help.
How long does this phase usually last?
It varies. But expecting a quick return to normal often creates more stress. Think in terms of gradual rebuilding, not instant recovery.
What kind of support helps after discharge?
Options that provide structured daytime care, clinical oversight, and consistent engagement tend to help most during this transition period.
You are not failing your child by feeling overwhelmed.
You’re responding to a situation that’s bigger than what one person can hold alone.
And the fact that you’re asking these questions—that you’re looking for something more—means you’re already doing something right.
Call 401-287-8652 or visit daytime treatment options to learn more about our partial hospitalization program services in Rhode Island.